What is diabetes? Types, symptoms, management, and the future of care
Diabetes is one of the most prevalent global health challenges of our time. According to the latest International Diabetes Federation Diabetes Atlas, 11.1% of adults, or roughly 1 in 9 people aged 20 to 79, are living with diabetes. This represents nearly 589 million individuals worldwide.
What is diabetes?
Diabetes is a disease that occurs when your blood glucose, also known as blood sugar levels, is too high. It occurs when your body either does not produce enough insulin or has become resistant to it and cannot effectively use the insulin it produces.
Insulin is a hormone that acts as a key, allowing glucose from your bloodstream to enter your body’s cells and be used as energy.
When this process is disrupted, glucose accumulates in your bloodstream instead of being absorbed by your cells. Over time, persistently high blood glucose levels can lead to serious complications affecting your heart, blood vessels, eyes, kidneys, and nerves. It has also been linked to some types of cancer, including liver, pancreatic, and colorectal cancer.
Types of diabetes
There are several types of diabetes. While each has different causes and characteristics, all involve challenges in regulating blood glucose levels.
Type 1 diabetes
Type 1 diabetes is an autoimmune condition in which your immune system mistakenly attacks the insulin-producing cells in your pancreas. As a result, your body produces little to no insulin, the hormone required to help glucose enter your cells and be used as energy.
It often develops in childhood or adolescence, although it can occur at any age. People with type 1 diabetes require lifelong insulin therapy to regulate their blood glucose levels. In 2025, an estimated 9.5 million people with type 1 diabetes. The majority of them live in high-income countries. Neither the cause nor the means to prevent type 1 diabetes is known.
Type 2 diabetes
Type 2 diabetes is the most common form of the condition, accounting for more than 90% of all diabetes cases. It typically develops through a combination of the following:
Your body’s cells become resistant to insulin, meaning they no longer respond effectively to the hormone. As a result, glucose cannot efficiently enter your cells and remains in your bloodstream.
Over time, your pancreas compensates by producing more insulin to overcome this resistance. However, this increased demand cannot be sustained indefinitely, and insulin production gradually declines. Eventually, your body does not produce enough insulin to maintain normal blood glucose levels.
Type 2 diabetes is strongly associated with lifestyle and metabolic risk factors, including physical inactivity and higher body weight. In many cases, it can be prevented or delayed through healthy lifestyle changes. Although it has historically been more common in adults, it is increasingly being diagnosed in younger populations. Note that, genetic predisposition and environmental factors also play an important role in the development of type 2 diabetes.
Gestational diabetes
Women of childbearing age are at an increased risk of diabetes during pregnancy. Across the world, about 1 in 6 pregnancies are affected by gestational diabetes (~16–17% of pregnancies/live births estimated).
This type of diabetes occurs during pregnancy and is similar to type 2 diabetes in that it involves insulin resistance. In many cases, it resolves after childbirth, but it increases the risk of developing type 2 diabetes later in life.
Gestational diabetes can affect both maternal and fetal health if not properly managed. With appropriate medical care, as well as healthy dietary and lifestyle adjustments, it can be effectively managed and, in some cases, the risks reduced.
What are the symptoms of diabetes?
Many people live with diabetes for years without knowing it. In fact, more than 4 in 10 cases globally remain undiagnosed. Recognising the symptoms early is critical, as earlier diagnosis significantly reduces the risk of long-term complications.
Common symptoms across type 1 and type 2 diabetes include:
- Increased thirst
- Frequent urination
- Unexplained fatigue
- Blurred vision
- Slow-healing wounds
- Recurring infections
Unintended weight loss is particularly associated with type 1 diabetes, where insulin deficiency leads to the breakdown of fat and muscle for energy.
Type 2 diabetes often develops gradually, and symptoms can be mild or absent in the early stages, which is why routine screening is important for those with risk factors such as higher body weight, family history, or age over 45.
Gestational diabetes typically presents with no obvious symptoms, making routine screening during pregnancy essential for early detection and management.
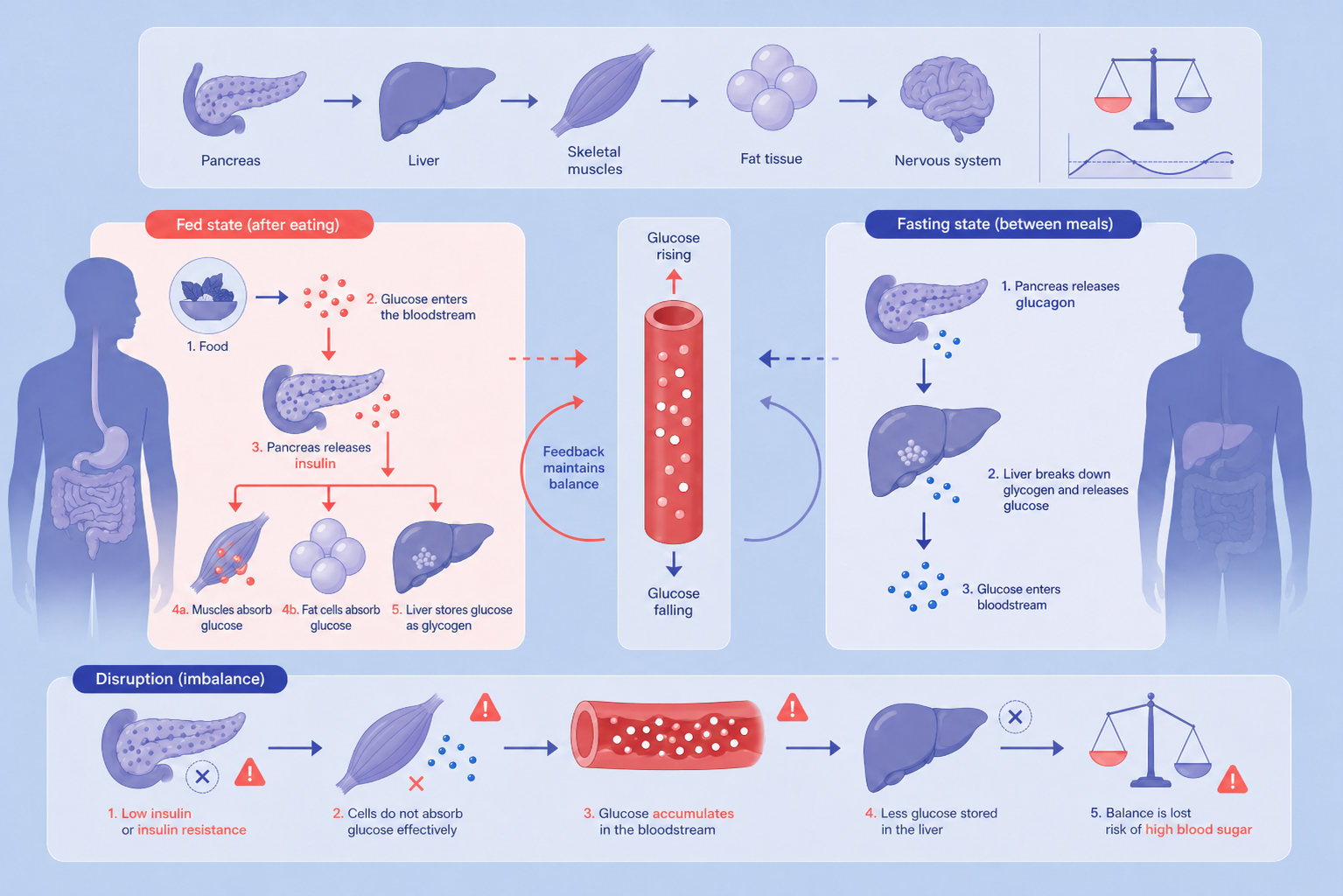
How does blood glucose regulation work?
Blood glucose regulation is a whole-body control system that keeps blood sugar levels within a narrow and healthy range.
The core goal is to balance glucose supply, from food and the liver, with glucose use by the body’s tissues. In healthy individuals, this feedback system maintains blood glucose levels at approximately 70 to 99 mg/dL, ensuring that the brain and other organs have a continuous energy supply, while preventing damage from levels that are too high or too low.
What health problems do people with diabetes develop?
People living with diabetes have a significantly higher risk of developing serious health problems, affecting the heart, blood vessels, eyes, kidneys, and nerves. In high-income countries, diabetes is a leading cause of cardiovascular disease, blindness, kidney failure, and lower limb amputation.
For instance:
- Cardiovascular disease is a major complication of diabetes, with people affected having about 2-4 times higher risk of events such as heart attack and stroke.
- Damage to small blood vessels in the eyes can lead to vision loss, with approximately 1 in 3 people with diabetes affected during their lifetime.
- Kidney disease is much more common, with the risk of kidney failure (end-stage renal disease (ESRD)) up to 10 times higher compared to people without diabetes.
Nerve damage, particularly in the lower limbs, can lead to loss of sensation and increase the risk of injury and infection. In severe cases, this may result in amputation, with a diabetes-related lower limb loss occurring somewhere in the world every 20 to 30 seconds.
Diabetes can also increase the risk of oral health problems, including gum disease, which is a major cause of tooth loss.
How to manage diabetes?
There is no cure for diabetes. With the right approach, however, people living with diabetes can maintain full, active, and healthy lives. Effective management focuses on controlling blood glucose, preventing complications, and tailoring care to your own needs.
Here is what the evidence shows works:
Monitor your blood glucose levels for short-term control
Blood glucose monitoring is a cornerstone of diabetes management. It provides immediate feedback on how your body is responding to your diet, physical activity, medications, or other underlying conditions. In this way, you get real-time data that allows you to be informed of a particular moment in time.
Traditionally, blood glucose levels have been measured using a blood glucose monitor, which requires pricking your finger, and collecting a tiny drop of blood that provides an instant reading.
More recently, commercially available continuous glucose monitoring (CGM) systems such as Dexcom G7 and Abbott FreeStyle Libre 3 Plus, have become increasingly important. These devices measure glucose levels continuously throughout the day and night, providing real-time data and revealing trends, patterns, and variabilities that single measurements may miss. By offering a more comprehensive view of glucose fluctuations, CGMs can support more precise and personalized diabetes management.
Monitor your HbA1c levels for long-term control
While blood glucose monitoring provides short-term insights, the HbA1c test reflects your average blood sugar levels over a longer period, typically the past two to three months.
HbA1c measures the proportion of hemoglobin in red blood cells that has glucose irreversibly attached to it. Because red blood cells circulate in the body for about 120 days, the level of HbA1c reflects cumulative exposure to glucose over time, with a stronger influence from more recent weeks. Unlike glucose monitoring, HbA1c does not measure blood sugar directly at a specific moment, but instead provides an overall picture of long-term glycemic control.
This makes HbA1c a key indicator in both the diagnosis and management of diabetes. Higher HbA1c values are associated with consistently elevated blood glucose levels and an increased risk of long-term complications.
However, HbA1c results must be interpreted carefully. Certain conditions that affect red blood cells, such as anemia, blood loss, or kidney disease, can influence results independently of actual blood glucose levels. As a result, HbA1c is most effective when used alongside regular blood glucose monitoring.
Together, these measures provide complementary insights: while blood glucose monitoring helps guide day-to-day decisions, HbA1c offers a broader, long-term perspective on diabetes management. In clinical practice, it is often complemented by continuous glucose monitoring metrics such as time in range (TIR).
Take control with lifestyle changes for effective diabetes management
Daily habits have a profound and measurable impact on your blood glucose. Research consistently shows that structured lifestyle changes can be as powerful as medication.
Eat smart, eat timed: Carbohydrates directly influence blood glucose, so identifying your personal tolerance using CGMs or post-meal monitoring is key. Studies show that insulin sensitivity is often higher earlier in the day, so prioritise carbohydrates earlier, keep evening meals lighter, and eat protein and vegetables before carbohydrates when possible. Avoid large, late suppers.
Move regularly: Aim for at least 150 minutes of moderate activity weekly. Post-meal physical activity, such as walking, has been shown to reduce postprandial glucose spikes, making it one of the most accessible habits for desk-based professionals
Quit smoking: Smoking raises blood glucose, worsens insulin resistance, and accelerates vascular damage. Quitting is one of the highest-impact decisions a person with diabetes can make, with measurable benefits beginning within weeks.
Prioritise sleep: Even one night of poor sleep temporarily reduces insulin sensitivity. Consistent sleep schedules, limiting screens before bed, and avoiding late meals all meaningfully support glucose control.
Manage stress: Stress triggers cortisol release, which raises blood glucose directly. Mindfulness, regular exercise, and structured breathing techniques have demonstrated measurable benefits for glycaemic outcomes.
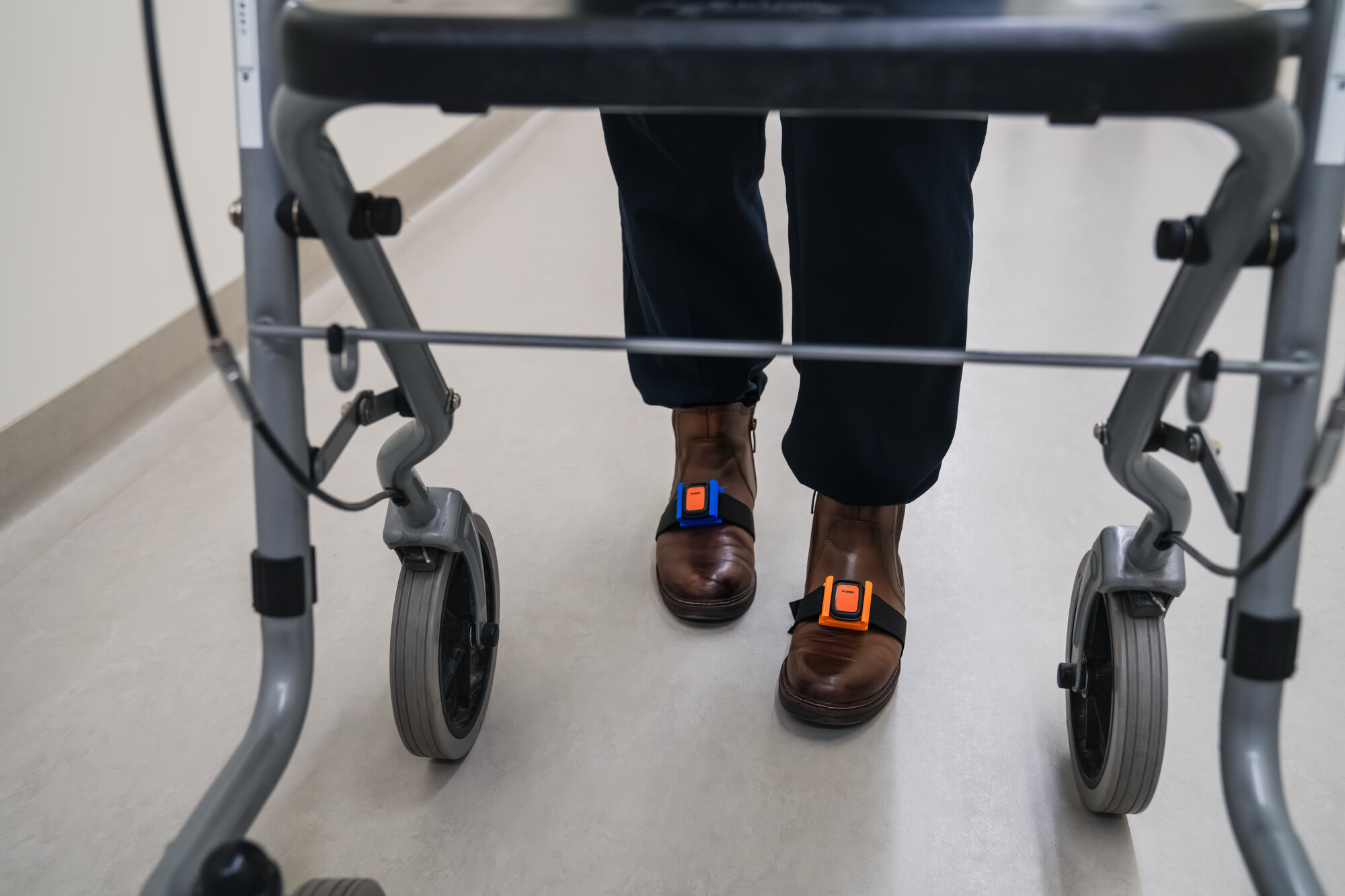
Protect your feet: High blood sugar reduces blood flow and can damage nerves in the feet, a condition called diabetic neuropathy. This causes pain, tingling, or loss of sensation. Without attention, minor cuts or blisters can develop into serious infections. Wash and dry your feet daily, moisturise regularly, and inspect them for sores, redness, or swelling. Never go barefoot, even indoors. If a wound does not begin healing within a few days, contact your healthcare professional promptly.
Care for your teeth: Diabetes raises the risk of gum disease and oral infections. Brush twice daily with fluoride toothpaste, floss daily, and attend dental check-ups at least twice a year. Bleeding, red, or swollen gums warrant a prompt call to your dentist.
Attend regular check-ups: Diabetes management extends beyond self-monitoring. Schedule two to four diabetes reviews per year alongside your annual physical. These visits allow your healthcare team to assess nutrition, activity, kidney function, nerve health, and cardiovascular risk, as well as examine your feet for any issues requiring treatment. An annual eye exam is equally important: early detection of retinal damage, cataracts, and glaucoma, all linked to diabetes, can prevent irreversible vision loss.
Take your medication as prescribed
Most people with diabetes require medication to manage their blood glucose levels. For type 1 diabetes, insulin therapy is essential, delivered via injections or an insulin pump. For type 2 diabetes, treatment typically begins with metformin, which reduces glucose production in the liver.
Where additional control is needed, newer drug classes have transformed the landscape: GLP-1 receptor agonists such as semaglutide support both glucose control and weight loss, while SGLT2 inhibitors offer added cardiovascular and kidney-protective benefits. Treatment is increasingly personalised, guided by individual risk factors, comorbidities, and real-world outcomes data.
What are the challenges in diabetes care today?
Despite advances in treatment, diabetes care remains complex. Access to insulin, continuous glucose monitoring (CGM), and specialist care is still unequal, particularly in low- and middle-income settings. Managing diabetes is also psychologically demanding, with higher rates of distress and depression that can negatively affect outcomes.
At a system level, clinical evidence from randomized controlled trials (RCTs) does not always reflect real-world populations, while fragmented health data limits long-term insights into disease progression. Key groups, such as older adults or people with multiple conditions, are often underrepresented, leaving gaps in the evidence needed to guide effective, personalized care.
To address these challenges, data-driven approaches such as real-world data are becoming increasingly important.
The role of real-world data in understanding diabetes
What is real-world data?
While clinical decision-making has traditionally relied on randomized controlled trials (RCTs), these studies often involve restricted populations and controlled settings that may not reflect everyday clinical practice.
Observational health studies using real-world data (RWD), such as electronic health records, claims data, and registries, offer a complementary approach. They provide insights into how treatments perform in routine care and are particularly valuable for answering questions that are difficult or impractical to study in clinical trials.
As a result, RWD is increasingly being used by clinicians, researchers, and regulators to inform decision-making and improve outcomes in diabetes care. Standardized data models such as OMOP enable consistent analysis across heterogeneous data sources.
Observational health studies in diabetes
A leading example is the LEGEND-T2DM study, a large-scale, federated analysis conducted within the OHDSI community. It compared the effectiveness and safety of second-line treatments for type 2 diabetes across 13 international databases, all standardized using the OMOP common data model.
By applying a consistent analytical approach across diverse healthcare systems, the study generated robust, reproducible real-world evidence at scale. It demonstrated that well-designed observational studies can complement, and in some cases approach the evidentiary strength of, traditional clinical trials, highlighting the increasing methodological rigor of real-world research.
Building on these advances, platforms like Data4Life’s Data2Evidence help enable collaborative research across institutions without requiring sensitive patient data to be shared. This supports faster, more transparent studies and accelerates the generation of evidence in diabetes.
The future of diabetes care
As healthcare data becomes more standardized through approaches like the OMOP common data model, it becomes easier to analyze information consistently across institutions. This improves data quality, enables interoperability, and lays the foundation for large-scale, reliable research in diabetes. Interoperability standards and common data models are key enablers of scalable, cross-institutional research.
Building on this foundation, advances in AI and digital health are helping translate real-world data into action. From earlier risk detection to more personalized treatment decisions, these technologies are enabling more proactive and tailored approaches to diabetes care.
Key takeaways
- Diabetes is a chronic condition requiring lifelong management
- Early detection and monitoring are critical
- Lifestyle changes significantly improve outcomes
- Real-world data is shaping the future of diabetes care
Together, these advances signal a shift toward more proactive, personalized, and data-driven diabetes care. At Data4Life, we are working to make that foundation stronger, enabling researchers, clinicians, and health systems to generate the evidence needed to transform diabetes care.
The contents of this article reflect the current scientific status at the time of publication and were written to the best of our knowledge. Nevertheless, the article does not replace medical advice and diagnosis. If you have any questions, consult your general practitioner.
Originally published on